You know that feeling when you’re sitting in a doctor’s waiting room, frantically trying to remember if you brought the right insurance card, wondering if you filled out the pre-visit forms correctly, and mentally calculating whether you’ll make it back to work in time for your 2 PM meeting? That’s not just appointment anxiety—that’s the weight of an entire invisible job you never applied for.
Health administration isn’t healthcare. It’s the sprawling, exhausting work that surrounds healthcare: the scheduling and rescheduling, the insurance calls, the form-filling, the prescription pickups, the follow-up appointments you’re supposed to remember to book, the test results you’re supposed to call about, the referrals you’re supposed to pursue. It’s a full-time job masquerading as “just taking care of yourself.”
And if you’re managing health admin for a family? Multiply that complexity by every person in your household, add coordination between providers, and throw in the emotional labor of being the one who remembers everyone’s medical history when they can’t.
The Three-Phase Health Admin Stack
The real scope of health administration becomes clear when you map out everything that happens before, during, and after any medical interaction.
The “before” phase starts weeks or months ahead of an appointment. You research providers, check insurance coverage, request time off work, arrange childcare. You fill out intake forms that ask for information you don’t have memorized, dig through old records to find previous surgery dates, and try to articulate symptoms that feel too vague or too embarrassing to describe accurately.
The “during” phase is deceptively simple—you show up and receive care—but even this requires mental bandwidth. You’re trying to remember the questions you wanted to ask, process new information, and make decisions while potentially feeling vulnerable or unwell.
The “after” phase is where the real administrative burden lives. You need to schedule follow-up appointments, fill new prescriptions, submit insurance claims, follow care instructions, and often coordinate with other providers. You’re supposed to monitor symptoms, track medication effects, and remember to call if things don’t improve within a certain timeframe.
Each phase generates its own set of open loops—things you need to remember, track, and follow up on. And unlike other types of administrative work, health admin comes with stakes that feel existential. Miss a work deadline and you might get a stern email. Miss a health follow-up and you might miss something serious.
Why Health Admin Breaks Us
Health administration is uniquely exhausting because it combines three of the most cognitively demanding elements: high stakes, radical uncertainty, and bureaucratic complexity.
The stakes feel enormous because they are. This isn’t about optimizing your calendar or streamlining your workflow—it’s about your body, your family’s wellbeing, your mortality. Every missed appointment or delayed follow-up carries the weight of “what if I’m making a mistake that matters?”
The stakes aren’t just high—they’re invisible until something goes wrong.
The uncertainty is relentless. You don’t know how long appointments will take, whether insurance will cover procedures, or when test results will come back. You can’t plan around healthcare the way you can plan around other commitments because the healthcare system operates on its own timeline, not yours.
The bureaucracy is deliberately obtuse. Insurance systems seem designed to exhaust you into giving up. Provider portals require different logins with different password requirements. Referral processes involve phone calls that transfer you between departments until you lose track of what you were trying to accomplish in the first place.
When you combine high stakes with uncertainty and bureaucracy, you get a perfect storm for anxiety and mental overload. You can’t just “set it and forget it” because too much could go wrong. But you also can’t control most of the variables, so you end up in a state of constant low-level vigilance.
The Spillover Effect
Health admin doesn’t stay contained within the healthcare system—it spills into every other area of life. You’re taking work calls while sitting in waiting rooms, rescheduling family commitments around medical appointments, and lying awake at night wondering if you remembered to call about those test results.
The cognitive load shows up at unexpected moments. You’re in the middle of a work project when you remember you need to schedule that follow-up appointment. You’re trying to plan a weekend trip when you realize you need to coordinate prescription refills. You’re having dinner with your family when you remember you never called the insurance company about that disputed claim.
For working parents, health admin becomes a coordination nightmare. You’re managing not just your own medical needs, but tracking pediatric appointments, school health forms, and family medical history. You become the keeper of everyone’s vaccination records, the one who remembers which child is allergic to which medication, the person who can recite insurance member numbers from memory.
The mental load multiplies when family members assume you’ll handle the health admin because you’ve always handled it. Partners might show up to appointments without knowing what insurance card to bring. Kids expect you to remember their medication schedules and dietary restrictions. Everyone assumes you’re tracking the family’s collective health needs because someone has to, and you’ve been doing it.
What Handoff Could Look Like
Imagine if health administration worked more like other professional services. You wouldn’t expect to remember your lawyer’s filing deadlines or track the status of your accountant’s work—you’d expect them to manage their own processes and keep you informed.
Real handoff in health admin would mean systems that hold context across time and providers. Instead of filling out the same medical history on fifteen different forms, your information would follow you. Instead of trying to remember whether you’re supposed to call about test results or wait for them to call you, the system would manage the follow-up loop.
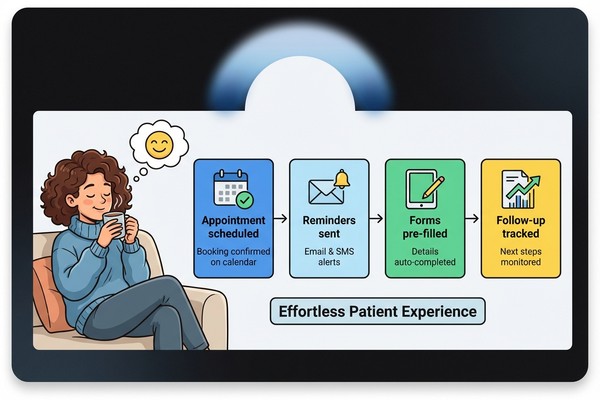
Practical handoff might include scheduling systems that actually coordinate with your calendar, not just their availability. Prescription management that tracks refills and alerts you before you run out. Insurance coordination that happens behind the scenes instead of requiring you to become an expert in medical billing codes.
The goal isn’t to remove you from health decisions—it’s to remove the administrative friction that makes healthcare feel like a second job. You’d still choose your providers, make treatment decisions, and stay informed about your care. You just wouldn’t have to project-manage the entire process.
Your Open Health Loops Right Now
Take a moment to mentally inventory your current health admin burden. What appointments do you need to schedule? What follow-ups are you supposed to remember? What forms are sitting half-completed on your desk? What insurance issues are you avoiding because they feel too complicated to tackle?
Most people are surprised by how many open health loops they’re carrying. There’s the specialist referral you never followed up on, the prescription that needs refilling, the test results you’re supposed to call about, the insurance claim you need to dispute. Each of these represents mental bandwidth you’re using to hold information that could be held elsewhere.
The exercise isn’t meant to overwhelm you—it’s meant to make visible the work you’re already doing. Once you can see the full scope of health admin in your life, you can start to imagine what it would feel like to hand some of it off.
A Care-Aware Approach
The solution to health admin overload isn’t just better organization or more efficient systems—it’s care-aware design that acknowledges the emotional and cognitive reality of managing health needs.
Care-aware systems would reduce stress by providing clear communication about next steps and timelines. Instead of wondering whether you’re supposed to call about results, you’d know exactly when and how you’ll hear back. Instead of trying to coordinate multiple appointments across different providers, scheduling would happen with awareness of your existing commitments.
Good health admin support doesn’t just track appointments—it holds the anxiety of remembering.
Care-aware systems would reduce forgetting by maintaining context across interactions. Your dietary restrictions, medication allergies, and family history would be available when needed without requiring you to recite them repeatedly. Care instructions would be delivered in formats that work for your life, not just printed on paper you’ll lose.
Care-aware systems would reduce rework by coordinating information between providers and insurance systems. You wouldn’t need to become a translator between different parts of the healthcare system because the systems would communicate with each other.
The goal is health admin that feels supportive rather than burdensome—systems that hold health context gently, without requiring you to become a healthcare project manager.
Beyond Individual Solutions
Health administration is exhausting because the current system is designed around institutional convenience, not human needs. Real solutions require more than individual optimization—they require systems that acknowledge health admin as legitimate work that deserves support.
Until those systems exist, the burden falls disproportionately on individuals and families who are already managing full lives. Recognizing health admin as a handoff candidate isn’t about finding the perfect app or developing better organizational skills. It’s about acknowledging that this work is real, it’s exhausting, and it deserves better support than “just remember to call your doctor.”
The first step is making the work visible. The second step is imagining what it would feel like to hold less of it yourself.
This article was created with collaboration between humans and AI—we hope you ❤️ it.
